Early Mobilization
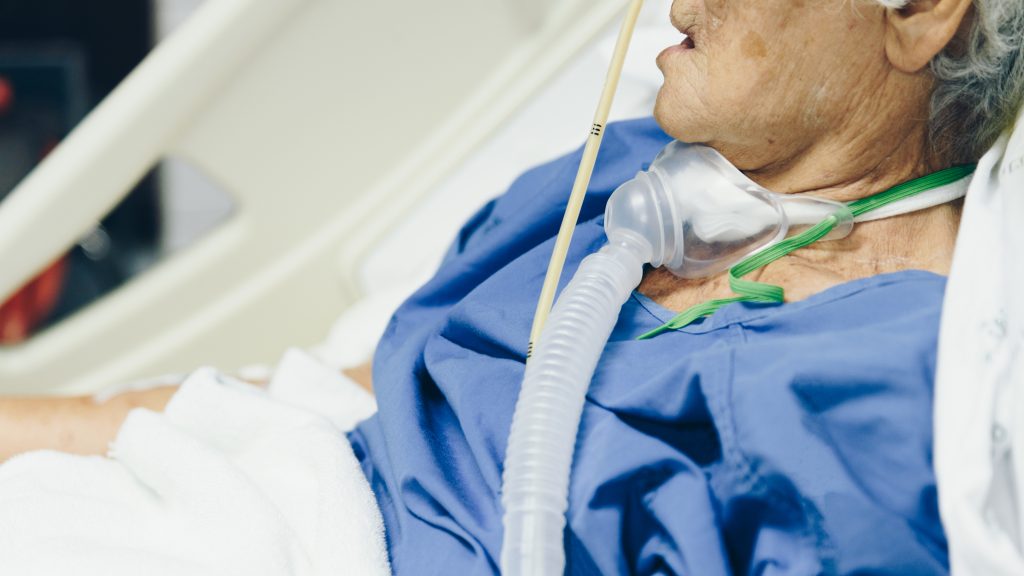
Early Mobilization for Patients with Tracheostomy and Mechanical Ventilation
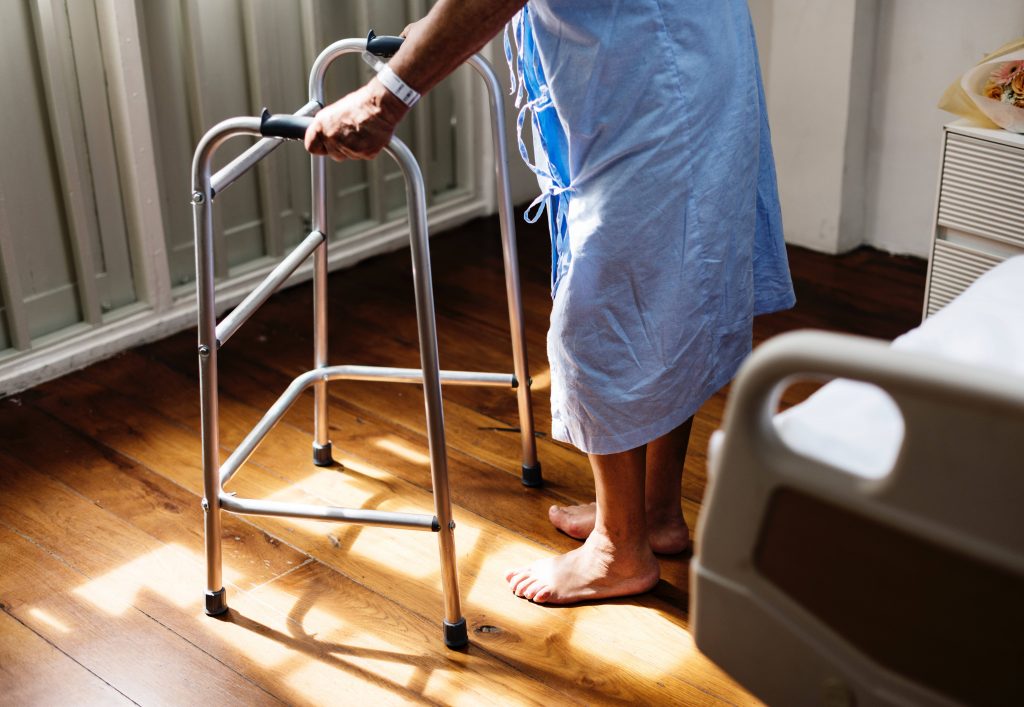
Early mobilization for patients with tracheostomy and mechanical ventilation can include activities such as sitting, standing and ambulation as well as passive exercises, like range of motion exercises and ergometry. Early mobilization is an important part of the rehabilitation process for individuals with tracheostomy in order to strengthen the patient and mobilize secretions. Airflow with a tracheostomy is redirected in and out of the tracheostomy tube, which bypasses the upper airway and vocal folds. Typical coughing for airway clearance is ineffective due to the open tracheostomy tube. Secretion management strategies including early mobilization are important for loosening and mobilizing secretions and preventing atelectasis and pneumonia.
Muscle disuse atrophy occurs in a significant proportion of critically ill patients. Critically ill patients who are on strict bed rest have a decline of 1% to 1.5% per day and up to 50% of total muscle mass in 2 weeks (Morris, PE, 2007). Profound neuromuscular weakness due to bedrest, immobility and critical illness may lead to physical impairment with over 50% of one-year survivors of prolonged mechanical ventilation needing assistance in basic activities of daily living (Choi, Tasota, & Hoffman, 2008). Intensive Care Unit Acquired Weakness (ICU-AW) describes a syndrome involving muscle wasting and is associated with higher mortality, poor patient outcomes and a delay of weaning process (Clarissa, C et al, 2019).
Critically ill patients are also at high risk for cognitive and psychological disabilities. Cognitive impairment, including impaired executive function, memory, language, and attention, is widespread; almost 80 percent of ICU survivors suffer from cognitive impairment early after discharge, with deficits often lasting from months to years (Hopkins, RO, Jackson, JC, 2009). The prevalence of psychiatric morbidity, including clinically significant depression, anxiety, and post-traumatic stress disorder, remains high among ICU survivors (Davydow DS et al, 2008).
The adverse sequelae from long term mechanical ventilation (infection, cognitive and psychological decline as well as neuromuscular dysfunction) precipitates longer hospital stays. Longer stays equate to higher hospital resources and higher economic burden on patients and hospitals.
Evidence suggests that early mobilization can help to mitigate the effects of physical, cognitive and psychological complications. Early mobilization has led to better outcomes than a control including shorter duration of delirium, more ventilator free days, better functional outcomes (Schweickert D et al, 2009, Li Z et al, 2019). Yet, despite the documented evidence that mobilizing patients early during ventilation results in such benefits, ICUs still perpetuate a culture of oversedation and bedrest for this vulnerable population.
Safety of Early Mobilization
Stable patients with tracheostomy and even on mechanical ventilation can participate in pulmonary rehabilitation and early mobilization to improve outcomes. Recent studies show that early rehabilitation is safe and feasible (Dong, Z et al, 2007). Early mobilization requires careful patient assessment and management and multidisciplinary team cooperation and education. Care should be taken and use of clinical expertise in assessing tracheostomy and ventilator dependent patients for candidacy for early mobilization.
The implementation of an early mobilization program requires a multidisciplinary approach, including collaboration between nurses, rehabilitation therapists, respiratory therapists, physicians, and administrators.
Video of a patient walking while on mechanical ventilation
Resources
Dong ZH, Yu BX, Sun YB, Fang W, Li L. Effects of early rehabilitation therapy on patients with mechanical ventilation. World J Emerg Med. 2014;5(1):48–52. doi:10.5847/wjem.j.1920-8642.2014.01.008
Li Z, Peng, Z, Zhu B, Zhang Y, Xi, X. Active mobilization for mechanically ventilated patients: a systematic review. Arch Phys Med Rehabil 2013 Mar;94(3):551-61. doi: 10.1016/j.apmr.2012.10.023.
Morris PE. Moving our critically Ill patients: mobility barriers and benefits. Critical Care Clinics. 2007;23(1):1–20. [PubMed] [Google Scholar]
Schweickert D, Pohlman M, Pohlman A, Nigos C, Pawlik A,,Esbrook, C, Spears L, Miller M, Franczyk M, , Deprizio D,Gregory A Schmidt G, Bowman A, Barr R, McCallister, Hall J, Kress J, Early physical and occupational therapy in mechanically ventilated, critically ill patients: a randomised controlled trial. The Lancet 2009; 373; 1874-1882