Preventing Infections in Patients with Tracheostomy

Preventing Infection in Individuals with Tracheostomy
Maintaining a high level of infection control is the responsibility of all health care staff working with any patient, particularly with individuals with tracheostomy and mechanical ventilation in order to ensure the safety of the patient, visitors and staff. Infection may be bacterial (gram negative organisms, Streptococcus pneumoniae, Haemophilus influenzae, Staphylococci and b Haemolytic Streptococcus Group A) or viral (respiratory synctial virus, parainfluenza) in nature.
Infection rates may be reduced with standard infection control procedures (hand hygiene, personal protective equipment), decontamination of respiratory equipment, reducing the potential for aspiration, reducing sedation needs, improving secretion management, and adequate tracheostomy cleaning and care. Weaning and decannulation will have the greatest impact on reducing the risk of infection.
Educate health care workers about infection control procedures and prevention methods to improve competency and adherence to hospital infection control procedures. Educate workers according to the worker’s level of responsibility in the health care setting and involve workers in the implementation of intervention to prevent infections by using performance improvement tools and techniques.
Common Pathogens
The infections most frequently associated with tracheostomy are either tracheobronchitis or mainly pneumonia, with up to 60% of hospitalized patients developing pneumonia (Ahmed, QA, 2001). Diagnosis of an infection is sometimes difficult because patients with tracheostomy are often colonized with potentially pathogenic bacteria. The diagnosis is often made on clinical features such as cough, purulent secretion, systemic signs of infection, impairments in gas exchange and the presence of an infiltrate on chest x-ray, should also be checked.
Gram-negative organisms are responsible for 50% of deep infections in patients with tracheostomies. Streptococcus pneumoniae, Haemophilus influenzae, Staphylococci and b Haemolytic Streptococcus Group A are also common causes of bacterial infection in the patient.
Risk Factors for Infection in Patients with Tracheostomy
There is a high susceptibility for infection in patients with tracheostomy due to the loss of function of the upper airway. With an inflated cuff, there is a loss of airflow through the upper airway. Some of the functions of the upper airway include condition of inspired air to body temperature and 100% relative humidity. Tracheostomy can lead to pathological changes of the lower airways, including damage to the ciliated tracheal mucosa, thickening of airway secretions, and the loss of mucociliary transport. Repeated cleaning and suctioning of the lower airway/the trachea is necessary, which results in significant patient discomfort and increases the risk of lower respiratory tract infection and airway obstruction. Other complications of the tracheostomy that may increase the risk of infection is that the patient may have poor secretion management and an increased risk of aspiration.
Fagon et al. suggested that the incidence of VAP increases by 1% per day of invasive mechanical ventilation. Risk factors associated with bacterial colonization include residing in a medical care home and the presence of a cuff (Lepainteur, M, 2019). The presence of a cuff has also been associated with increased respiratory infections (Hernandez, 2012). Respiratory secretions pool around the cuff of the tracheostomy tube and will gradually leak past the cuff down into the lungs. Gastric contents, heavily colonised with Gram-negative organisms may also be aspirated into the lungs. The cuff also reduces the ability for the patient to effectively clear secretions above the cuff.
Other general risks include poor overall health and oral hygiene.
- Patients in healthcare who have underlying medical conditions such as diabetes, cancer, and organ transplantation are at increased risk for infection because often these illnesses decrease the immune system’s ability to fight infection.
- Certain medications used to treat medical conditions, such as antibiotics, steroids, and certain cancer fighting medications increase the risk of some types of infections.
- Lifesaving medical treatments and procedures used in healthcare such as urinary catheters, tubes, and surgery increase the risk of infection by providing additional ways that germs can enter the body. The tracheostomy tube may be a conduit for germs through the open tracheostomy tube.
- Poor oral care is associated with infection from aspiration of bacteria in the oral cavity.
Ventilator Associated Pneumonia
The definition of ventilator associated pneumonia has been debated in the literature. A particular difficulty with many commonly-used VAP definitions, including the NHSN PNEU definitions (revised in 2002), is that they require radiographic findings of pneumonia. Evidence suggests that chest radiograph findings do not accurately identify VAP. The subjectivity and variability inherent in chest radiograph technique, interpretation, and reporting make chest imaging ill-suited for inclusion in a definition algorithm to be used for the potential purposes of public reporting, inter-facility comparisons, and pay-for-reporting and pay-for-performance programs.
In 2011, the Centers for Disease control established a new approach to surveillance of Ventilator Associated Events (VAE). There are three definition tiers within the VAE algorithm:
- Ventilator-Associated Condition (VAC)
- Infection-related Ventilator-Associated Complication (IVAC)
- Possible VAP (PVAP).
Risk Factors for Ventilator Associated Pneumonia
Risk factors for VAP (Nseir, 2007; Koenig, S & Truwit, J, 2006):
Host related risk factors:
- Neurological injury
- Corticosteriod Use
- Gastric PH-modifying agents
- Medical history and underlying illness
- Male gender
- Extreme age
- Prior central nervous system disorder
- Immunocompromised
- Acute underlying diseases
- Emergent surgery
- Neurosurgery, theracic surgery and cardiac surgery
- Burns
- Re-intervention
- Acute severity factors
- Organ system failure index of at least 3
- Acute renal failure
- Acute respiratory distress syndrome
- ECMO, intra-aortic support
- Ulcer disease
- Duration of intubation and mechanical ventilation
- Reintubation
- Supine positioning during enteral feedings
- Enteral nutrition
- Antibiotic use
- Poor infection control conditions
- Contaminated respiratory equipment, medications, or water
- Absence of subglottic secretion drainage
- Frequent vent circuit changes
Standard Infection Control Methods
Infection control prevents the spread of infection. Standard Precautions apply to 1) blood; 2) all body fluids, secretions, and excretions, except sweat, regardless of whether or not they contain visible blood; 3) non-intact skin; and 4) mucous membranes. Standard precautions are designed to reduce the risk of transmission of microorganisms from both recognized and unrecognized sources of infection in hospitals. Standard precautions includes the use of: hand hygiene and appropriate personal protective equipment.
Hand Hygiene
Microbes are acquired on the skin from direct contact with people, surfaces and the environment and is the mode of spread for the majority of health care associated infections. Hand hygiene reduces the risk of transmission of infection from patient to patient as well as to the healthcare worker. It has also been shown to reduce morbidity, mortality and costs associated with health care associated infections (CDC, 2002). Hand hygiene is a simple, yet effective way to prevent the spread of disease. Contaminated hands or equipment can pose a threat to patients with tracheostomy, who are specifically susceptible at tracheostomy wound sites, during tracheostomy care or suctioning.
If hands are visibly dirty or if the patient has a C. difficile infection, the hands should be washed with soap and water. Hands should be washed thoroughly, at least 15 seconds, making sure all parts of the hands are clean. The thumb, fingertips and between the fingers are the most often missed areas. If the hands are not visibly dirty, alcohol based hand sanitizer is the preferred method of cleaning. Compared to soap and water, alcohol based hand sanitizer is more effective at killing potentially deadly germs on hands, requires less time, is more accessible, produces reduced bacterial counts on hands, and improves skin condition with less irritation and dryness (CDC, 2019). Hand hygiene should be performed whether or not gloves are worn.
However, despite the evidence that hand hygiene prevents the spread of infection, healthcare worker adherence to hand hygiene protocols has been poor.
Use of Personal Protective Equipment
Personal protective equipment (PPE) such as gowns, gloves, masks, and goggles protect the patient from infection from other patients and also help to protect the healthcare worker. The use of gloves is a standard precaution for all patient care. Glove use is not an alternative for hand washing. Hands should be washed before placing gloves and after removal.
The type of protective equipment used should be ascertained by risk assessment of known or suspected infections, the procedure to be performed and the anticipated degree of contact with blood or body fluids. When involvement with respiratory secretions from a patient is anticipated, wear a gown and change it after soiling occurs and before providing care to another patient. During suctioning with an open suction catheter, consider use of a gown and protective eye wear in addition to gloves, particularly if the patient has an infection or copious secretions.
Transmission-Based Precautions (i.e., Airborne Precautions, Droplet Precautions, and Contact Precautions), are recommended to provide additional precautions beyond Standard Precautions to interrupt transmission of pathogens in hospitals.
- Airborne Precautions used for infections spread in small particles in the air such as chicken pox.
- Droplet Precautions used for infections spread in large droplets by coughing, talking, or sneezing such as influenza.
- Contact Precautions used for infections spread by skin to skin contact or contact with other surfaces such as herpes simplex virus.
Tracheostomy Specific Concerns for Infection
Tracheostomy Stoma Infection

The incidence of tracheostomy stoma infection varies from institutions. Stoma infections can occur following the tracheotomy procedure, but may be reduced following percutaneous dilational tracheotomy procedures (PDT). Following surgical tracheotomy, rates vary between 0-63%, while PDT rates have been between 0-10% (Durbin, 2005). The site should be inspected daily for signs of infection. Signs of tracheostomy stoma infection include erythematous change, swelling around wound, purulent discharge from wound and discharge culture with bacterial growth. The patient may also complain of pain at the tracheotomy site.
It is important to keep the stoma site dry and free of secretions as moisture can predispose the patient to infection and skin breakdown. See Stoma Care for more information.
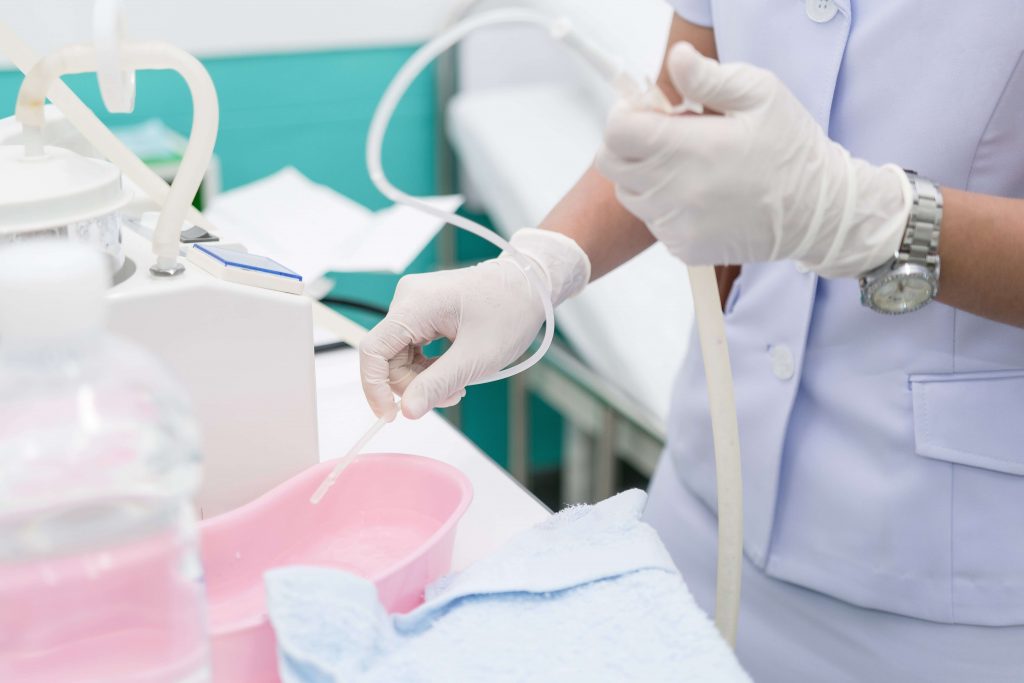
Tracheostomy Suctioning
There are open or closed suction catheters. No recommendation can be made for the preferential use of either the multi-use closed-system suction catheter or the single-use open-system suction catheter for prevention of pneumonia (CDC, 2003). If the open-system suction is employed, use a sterile, single-use catheter (CDC, 2003). During use of an open suction catheter, if the healthcare workers hands are contaminated and touch the suction catheter, bacteria can easily be transmitted. With an open suction catheter, secretions can easily be expelled out the tracheostomy tube and contaminate the health care worker and the environment. Suctioning therefore will require gloves, possibly a protective apron and staff may consider a mask and eye protection necessary if the patient is suffering from an infectious condition, or there are copious secretions which may result in splashing or aerosol spray.
Closed suctioning is recommended for patients with mechanical ventilation to prevent disconnection from the ventilator which can result in atelectasis. Disconnections also may allow for foreign objects including bacteria to contaminate inside the tracheostomy tube. Closed suctioning can reduce the healthcare workers exposure to sputum. The CDC (2003) does not have a recommendation about the frequency of routinely changing the in-line suction catheter of a closed-suction system in use on one patient.
For suctioning procedures and more information, please see Tracheostomy Suctioning.
Suctioning of the oral cavity with a suction catheter or Yankaeur suction can be included in a comprehensive oral hygiene program to reduce or prevent oral colonization of bacteria.
Tracheostomy Tube Care
Proper care including cleaning of the inner cannula and routine tracheostomy tube changes are important in preventing infections. Hand hygiene should be performed before and after tracheostomy tube care. When changing a tracheostomy tube, wear a gown, use aseptic technique, and replace the tube with one that has undergone sterilization or high-level disinfection.
Humidification and Nebuilizer Treatments
Individuals with tracheostomy have a loss of airflow through the upper airway, and therefore are unable to humidify and filter the lower airway sufficiently. Ciliated epithelial cells are the basis of mucociliary transport in the upper and lower airway. Their primary task is the elimination of dust and inhaled particles by transporting debris in a layer of mucus with a fast and synchronous ciliary beat frequency (CBF).
Artificial humidification such as HMEs and heated humidification are a standard of care for individuals with tracheostomy to compensate. In a prospective comparison of heated humidification to HME use, the patients using heated humidification required 40% less suctioning which may have been due to an increased number of ciliated epithelial cells in that group following heated humidification (Birk, R., 2013).
Humidifiers and nebulizer treatment are particularly vulnerable to colonization by Gram negative bacteria. Single use nebulizers may reduce this risk. If multidose medication vials are used, follow manufacturers’ instructions for handling, storing, and dispensing the medications. Between treatments on the same patient, rinse the nebulizer out with sterile water and dry thoroughly after each use. The fluid should be dispensed aseptically (CDC, 2003).
Breathing circuits with humidifiers:
- Breathing circuits should not be changed routinely. Only change the circuit when visibly dirty or. malfunctioning
- Periodically drain and discard any condensate that collects in the tubing of a mechanical ventilator, taking precautions not to allow condensate to drain toward the patient.
- Use sterile (not distilled, nonsterile) water to fill bubbling humidifiers.
- No recommendation can be made for the preferential use of a closed, continuous-feed humification system (CDC, 2004).
Ventilator breathing circuits with HMES:
- No recommendation can be made for the preferential use of either HMEs or heated humidifiers to prevent pneumonia in patients receiving mechanically assisted ventilation.
- Do not routinely change an HME more frequently than every 48 hours.
- Do not routine change (in the absence of gross contamination or malfunction) a breathing circuit that is in use by a patient more frequently than every 48 hours (CDC, 2003). Changing the ventilator circuit only when clinically indicated such as visible soiling or when faulty, does not increase the incidence of VAP and would result in significant cost savings compared to routine changing of circuit (Intensive Care Society, 2013).
Sedation
Sedation of endotracheally intubated patients is universal to ensure patient comfort. Continuous sedation can lead to accumulation of sedatives and over-sedation, and is associated with increased duration of mechanical ventilation Since intubation and mechanical ventilation predisposes patients to VAP, reducing the duration of mechanical ventilation should reduce that time at risk for developing VAP. Two strategies that have been used to reduce the duration of mechanical ventilation are daily sedation interruption (DSI) and daily spontaneous breathing trials (SBT). According to the Intensive Care Society, there is sufficient evidence to support the use of daily sedation interruption to prevent over-sedation and liberation from mechanical ventilation through daily spontaneous breathing trials (Hellyer, et al, 2016).
Long periods of sedation can impair pharyngeal function, airway protection and coordination of breathing and swallowing (Hardemark Cedbard, A, 2015). Sedation also causes prolongation of the timing for initiation of the swallowing reflex and a decrease in the number of swallows elicited (Nishino et al., 1987). Muscle atrophy can occur from limited use of the muscles for swallowing. Reduction in sedation may also allow for early intervention of swallowing therapy to reduce muscle disuse and aspiration risk.
Precautions for Prevention of Aspiration
The Center for Disease Control, in the Guidenline for Prevention of Healthcare Associated Pneumonia, the following is recommended:
As soon as the clinical indications for their use are resolved, remove devices such as endotracheal, tracheostomy, and/or enteral (i.e., oro- or nasogastric or jejunal) tubes from patients
Having a tracheostomy tube is a risk factor for aspiration with the potential to lead to the development of pneumonia. Food, liquid, and secretions are able to pass around the tracheostomy tube cuff and into the lower airways. Patients with an inflated cuff are at high risk of aspiration. See the Swallowing Management of Individuals with Tracheostomy page for more information about preventing aspiration and dysphagia management.
In a randomized study, those with the cuff deflated weaned quicker and had significantly less respiratory infections than those in the cuff inflated group (Hernandez et al, 2012). Prior to deflating the cuff of the tracheostomy (or endotracheal tube), suctioning should be performed to reduce the risk of aspirated secretions from entering the lower airways.
Decannulation is recommended as soon as feasible, if it can be achieved safely. Cuff deflation is an important step in the decannulation process.
Prevention of Aspiration with Endotracheal Tube
If feasible and not medically contraindicated, the use of non-invasive ventilation to reduce the need of endotracheal intubation or for weaning purposes can reduce aspiration pneumonia risks. Unless contraindicated, orotracheal intubation rather than nasotracheal intubation also reduces pneumonia rates. The use of an endotracheal tube with a dorsal lumen above the endotracheal cuff to allow drainage (by continuous or frequent intermittent suctioning) of tracheal secretions that accumulate in the patient’s subglottic area may also reduce VAP. Prior to cuff deflation for extubation, use of a subglottic suctioning may reduce aspirated secretions from entering the lungs. Also avoiding repeat endotracheal intubation in patient who have received mechanical ventilation (CDC, 2003). Repeated intubations increase the likelihood of damage to the vocal fold and surrounding mucosa, which increases aspiration risk.
Once intubation has occurred the focus of reducing risk of VAP should be at reducing colonization and aspiration (Koenig, S & Truwit, J 2006) to reduce the risk of pneumonia. Fagon et al. suggested that the incidence of VAP increases by 1% per day of invasive mechanical ventilation. Intubated patients may be more prone to develop VAP as compared to those with a tracheostomy because the ETT keeps the trachea and the oropharynx in communication, acting as a bridge for bacteria to move toward the dependent airways.
VAP rates are likely high in individuals with both endotracheal tubes and tracheostomy tubes due to medical fragility as well as the interference of normal physiological mechanisms to clear the airway of bacterial contaminants. With an inflated cuff, the individual is unable to produce an effective cough reflex. Tracheostomy allows for better oral hygiene as well as the possibility of cuff deflation to begin re-establishing airflow and use of the vocal folds. Tracheostomy may also allow for faster weaning from mechanical ventilation. However, VAP has not been shown to be different in early versus late tracheostomy (Terragni, 2011).
Prevention of Aspiration with Enteral Feeding Tube
Patients with tracheostomy and/or mechanical ventilation are at high risk of aspiration, even if an enteral feeding tube is in place. Enteral feeding includes nasogastric, gastrostomy, and jejunal tubes. When a nasogastric tube is initially placed, verify appropriate placement with a chest x-ray. Colorimetric capnography is another valid method for verifying NG tube positioning in mechanically ventilated patients.
Aspiration can occur from reflux or vomitus of enteral feeding. To prevent aspiration, elevate the head of the bed at an angle of 30-45 degrees, unless contraindicated by medical conditions(s). No recommendation for preferential use of small bore feedings, continuous versus intermittent or placing feeding tubes distal to the pylorus (CDC, 2004).
In terms of nasogastric tubes, the presence of a NGT has been associated with difficulty swallowing. In a 15 elderly individuals with normal swallowing, NGT increased airway penetration-aspiration (fine bore NGT with serial liquid swallows and puree) (ii) increased pharyngeal residue in the pyriform sinus (fine bore NGT with puree) and in the valleculae (both fine and wide bore NGT with soft solids) and (iii) an increase in pharyngeal transit duration regardless of consistency with longest swallowing durations with the widest tube (Pryor, 2015). Similarly, in young normals, the presence of a wide-bore nasogastric tube caused significant duration changes in several swallowing measures, namely duration of stage transition, duration of pharyngeal response, duration of pharyngeal transit, and duration of upper esophageal sphincter opening. Similar trends were seen for the fine-bore tube (Huggins, PS, 1999).
Prevention of oropharyngeal colonization
The literature shows a strong correlation between oropharyngeal bacterial colonization and presence of causative bacteria of VAP. Oral hygiene care is critical in reducing oropharyngeal colonization of bacteria and reducing ventilator associated pneumonia. Develop and implement an oral hygiene program which includes use of an antiseptic agent. Mori et al. (2006) compared two large groups of ICU, mechanically ventilated patients. Twelve hundred and forty eight patients received prescribed oral care three times daily. Six hundred and thirty seven patients had not received oral care during an earlier hospital period of stay and were used as historical controls. The incidence of VAP was significantly reduced for the oral care group compared to the non-oral care control group (3.9 versus 10.4).
Chlorhexidine oral rinse is an antimicrobial rinse which has widely been included as part of the routine oral care program for patients with tracheostomy and or mechanical ventilation, however the impact has been debated. Results from a Cochrane Review (2016) indicated that randomized controlled studies demonstrated chlorhexidine mouthwash or gel, reduces the risk of VAP compared to placebo or usual care from 24% to 18%. An updated meta-analysis focusing on double-blind studies in non-cardiac surgery patients showed that it had no impact on VAP rates or duration of mechanical ventilation or duration of ICU stay (Klompis, 2017). It is still widely used in VAP protocols for the intubated patient.
Hospitals are also including VAP bundles that include oral hygiene. In a study showing reduced VAP rate after implementing a VAP bundle that included head elevation, oral chlorhexidine gel, sedation interruptions and a ventilator weaning protocol (Moris, AC et al, 2011).
Prevention of Gastric Colonization
The CDC (2003) does not have a recommendation for the preferential use of sucralfate, H2-antagonists, and/or antacids for stress-bleeding prophylaxis in patients receiving mechanically assisted ventilation. There is also no recommendation by the CDC for the routine selective decontamination of the digestive tract of all critically ill, mechanically ventilated, or ICU patients or routinely acidifying gastric feedings. The Intensive Care Society (ICS) (2016) also indicates that there is insufficient evidence to give a clear recommendation of the use of gastrointestinal stress ulcer prophylaxis and the potential protective benefits of enteral feeding. The ICS recommend consideration of the risk profile of GI bleeding in each patient with judicious use of gastrointestinal stress ulcer prophylaxis in patients considered to be at risk of GI bleeding.
Summary
Patients with tracheostomy and/or mechanical ventilation are at high risk for infection. Health care workers should be educated on standard infection control methods (hand hygiene, personal protective equipment) as well as specific methods for these high risk patients including suctioning procedure, tracheostomy tube care, humidification, equipment cleaning, oral care, sedation interruption, and, if feasible, weaning and decannulation. Protocols for each method are recommended to standardize the approach in each facility.
For Covid-19 specific infection control recommendations please check our article, Covid-19 Tracheostomy and Mechanical Ventilation. The CDC and WHO also have recommendations regarding Covid-19 that are rapidly changing.
What to Read Next on Tracheostomy Education
Resources:
Birk R, Händel A, Wenzel A, et al. Heated air humidification versus cold air nebulization in newly tracheostomized patients. Head Neck. 2017;39(12):2481–2487. doi:10.1002/hed.24917
Durbin CG. Early complications of tracheostomy. RespirCare 2005; 50: 511-5.
Hellyer, TP, Ewan, V, Wilson, P, & Simpson, AJ (2016). The Intensive Care Society recommended bundle of interventions for the prevention of ventilator-associated pneumonia. Journal of the Intensive Care Society, 17(3), 238–243. https://doi.org/10.1177/1751143716644461
Huggins, P., Tuomi, S. & Young, C. Dysphagia (1999) 14: 157. https://doi.org/10.1007/PL00009598
Lepainteur, M et al. Risk factors for respiratory tract bacterial colonization in adults with neuromuscular or neurological disorders and chronic tracheostomy. Respiratory Medicine, Volume 152, 32 – 36
Mori, H., Hirasawa, H., Oda, S. et al. Intensive Care Med (2006) 32: 230. https://doi.org/10.1007/s00134-005-0014-4
Pryor, Lee N. et al. Impact of nasogastric tubes on swallowing physiology in older, healthy subjects: A randomized controlled crossover trial. Clinical Nutrition, Volume 34, Issue 4, 572 – 5
Terragni PP, Antonelli M, Fumagalli R, et al. Early vs Late Tracheotomy for Prevention of Pneumonia in Mechanically Ventilated Adult ICU Patients: A Randomized Controlled Trial. JAMA. 2010;303(15):1483–1489. doi:10.1001/jama.2010.47
Timsit JF, Esaied W, Neuville M, Bouadma L, Mourvllier B. Update on ventilator-associated pneumonia. F1000Res. 2017;6:2061. Published 2017 Nov 29. doi:10.12688/f1000research.12222.1









Responses