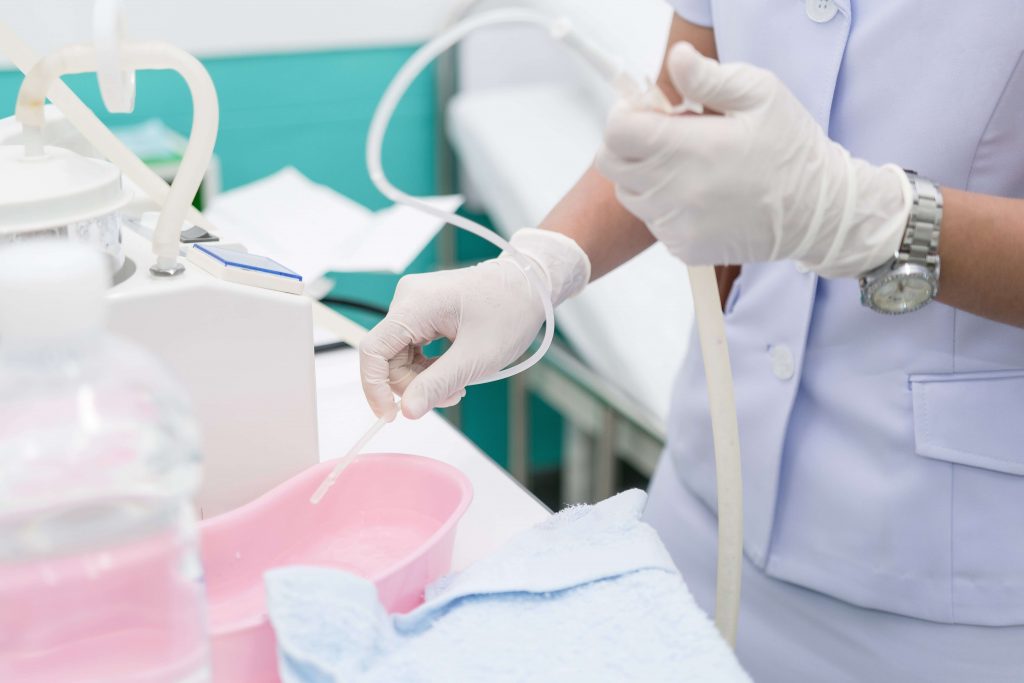
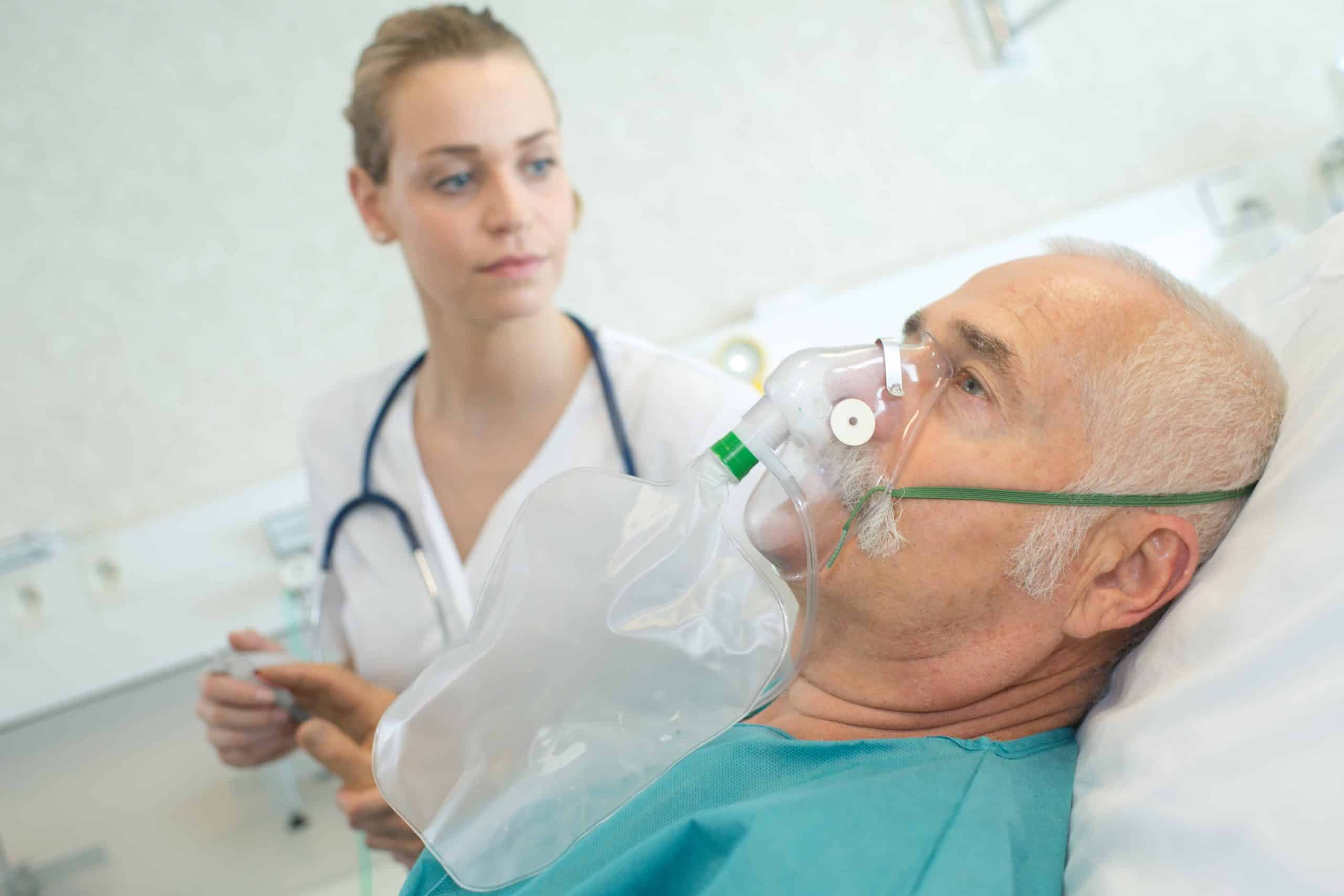
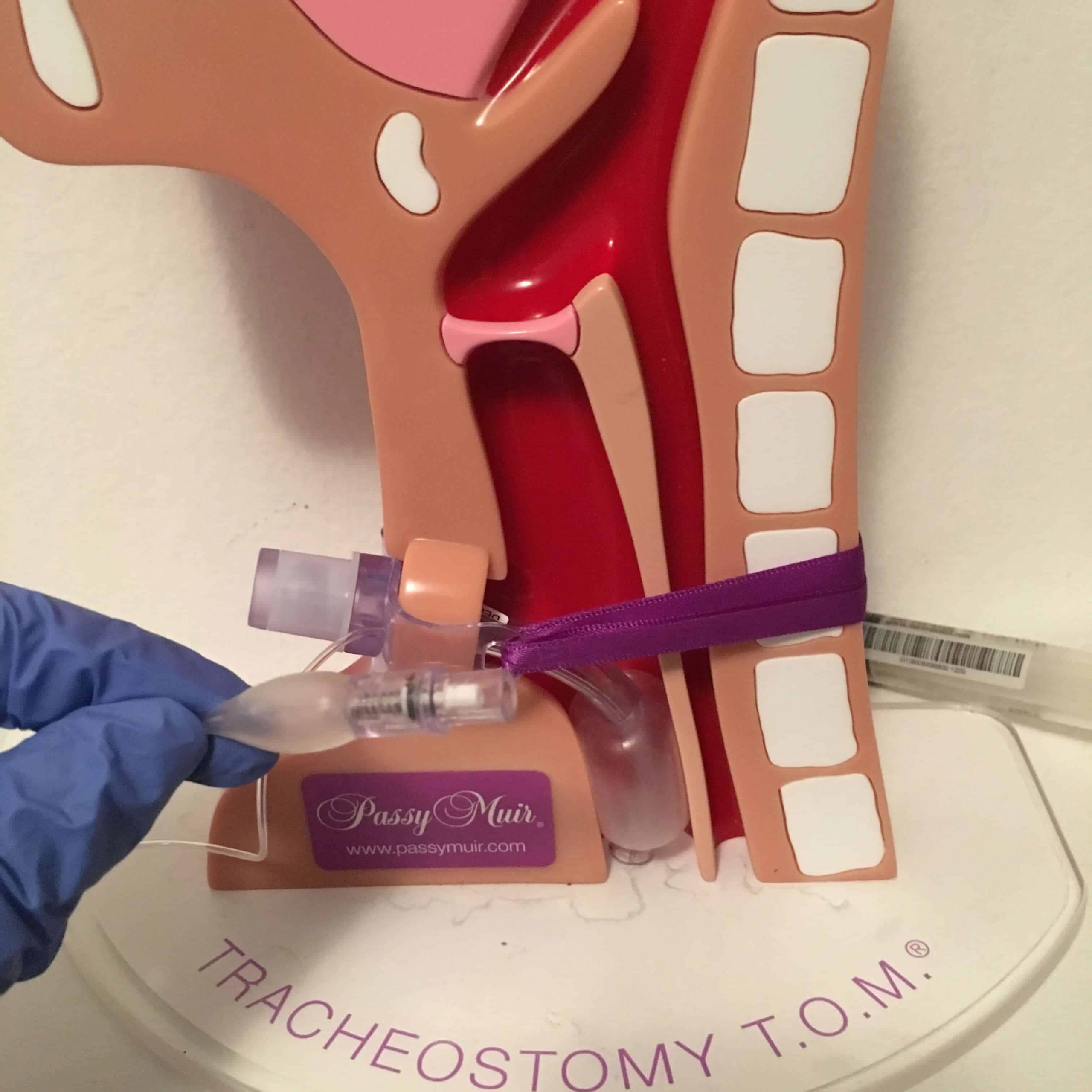
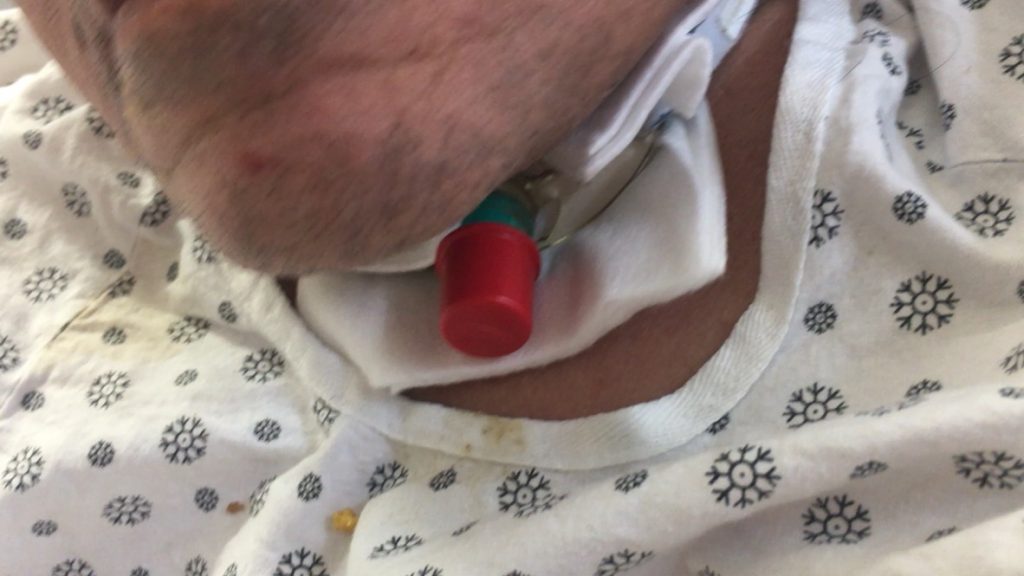
The normally closed respiratory system can be considered as “open” due to the tracheostomy tube, allowing air to escape from the tube. Airflow is redirected and bypasses the upper airway, which normally warms and filters the air. The air is typically drier and cooler when moving through a tracheostomy tube, which can lead to secretion retention. The lack of airflow through the upper airway also results in reduced sensation in that area. If the individual does not feel the secretions in the airway, secretions build up and stagnate. A general reduction in swallowing of secretions leads to muscle disuse which furthers escalates the cycle of impaired secretion management for tracheostomy patients. The tracheostomy tube is also a foreign object, and the body responds by producing more secretions.
The cough reflex is also impaired due to the open tracheostomy tube and lack of airflow through the upper airway. The cough reflex is vital in mobilizing secretions and acts as a protective mechanism to remove of foreign material from the airway. Subglottic pressure was measured with an open tracheostomy tube and found to be 0cmH20 (Gross, R). Subglottic pressure is required to produce an effective cough. Furthermore, individuals with tracheostomy may also have retained secretions and poor coughing due to muscle weakness and general immobility. Finally, patients may be on fluid restrictions which can further thicken secretions. All of these can contribute to the need to provide assistance in secretion management for individuals with tracheostomy.