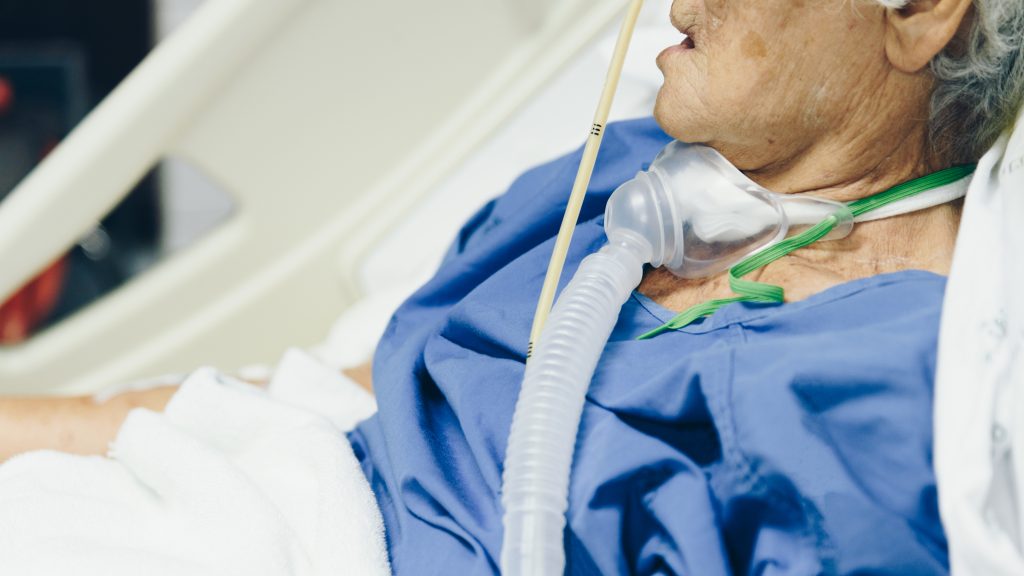
Tracheal Suctioning
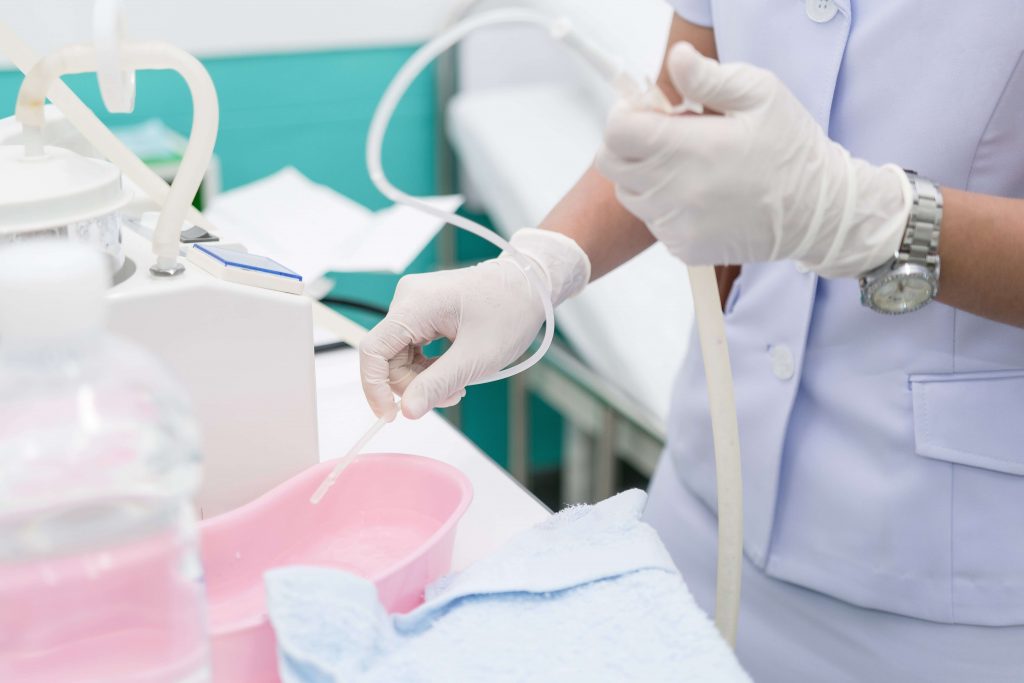
Tracheal Suctioning
The tracheostomy effects the normal functions of the upper airway including secretion management and humification due to impaired cough reflex, increased mucous production and impaired actions of the cilia. Tracheal suctioning is one strategy to assist in secretion management for individuals with tracheostomy. Suctioning is an important part of care for both the individual with tracheostomy as well as laryngectomy.
Tracheal suctioning is performed to remove secretions from the tracheostomy tube and airway in order to maintain a patent airway and avoid tracheostomy tube blockages. The amount of secretions varies by patient as does the amount of suctioning needs. Some individuals are able to project mucous out of the tracheostomy tube by coughing. Once an individual can tolerate a speaking valve or cap, they may be able to cough secretions around the tracheostomy tube, through the upper airway and out of the mouth. The ability to forcibly cough secretions through the upper airway is one indicator for readiness of decannulation.
Suctioning is a lifesaving procedure requiring timely and precise methodology. If done appropriately with caution, it decreases the risk of infection, pooling of secretions, and prolonged hypoxia. Suctioning of the airways should be performed by a skilled personnel with appropriate preparation to prevent complications of suctioning.
When to perform tracheal suctioning
The Clinical Consensus Guidelines indicates that the stoma and tracheostomy tube should be suctioned when there is evidence of visual or audible secretions in the airway, suspected airway obstruction, and when the tube is changed or the cuff deflated (Mitchell, 2013). Indications include noisy or moist respirations, prolonged expiratory breath sounds, increased respiratory effort, oxygen desaturations, restlessness, increased coughing or reduced effectiveness of coughing, increased use of accessory muscles and patient request. Signs of airway obstruction include hypoxia and cardiovascular changes. Easy passage of a suction catheter and removal of secretions confirms proper placement and patency of the tracheostomy tube.
There is no clear consensus on how frequently an individual should be suctioned. It is patient dependent on the amount of secretions and their ability to clear the secretions independently. Airway patency can be checked by attempting suctioning at least every 8 hours.
There are no absolute contraindications to suctioning. Risks are associated with suctioning and should be weighed with specific individual patient needs.
Possible complications of suctioning
Complications from suctioning are relatively uncommon if performed with care and pre-oxygenation prior to suctioning.
Complications of suctioning can include:
- Hypoxemia may result as some oxygen provided to the patient may be taken from the vacuum created during suctioning, resulting in less available oxygen. Reducing suctioning times to less than 15 seconds can prevent hypoxemia. Hypoxemia can also result from stimulation of the vagal nerve.
- Atelectasis can occur as the alveoli may close and be unavailable for gas exchange
- Cardiac dysrhythmia from the act of suctioning may disrupt the patient’s heart rhythm with bradycardia from stimulation of the vagal nerve.
- Bleeding can occur if there is trauma from the suction catheter to the tracheal wall. Large quantities of blood should be investigated as to the cause of the bleeding.
-
Infections may result from the possible introduction of bacteria into the respiratory tract if proper suctioning techniques are not performed.
-
Pain and discomfort can result from suctioning.
-
Anxiety can be associated with suctioning.
Trauma may be prevented through an appropriately sized catheter and proper suctioning technique with pressures not exceeding -150 mmHg (-20kPa) . Removal of a fenestrated inner cannula with placement of a non-fenestrated inner cannula prevents the suction catheter from passing through the fenestrations, which can cause trauma to the tissue.
There are no absolute contraindications to tracheal suctioning as problems are usually short lived and related to the baseline stability of the patient.
What to do when a suction catheter cannot be passed
Inability to pass the suction catheter is a red flag and indicates that the airway is not patent. An obstruction of the tracheostomy tube may be due to thick secretions or blood. The catheter may also not pass if the tube is dislodged. It is difficult to discern the exact reason.
First the inner cannula (if present) should be removed. Some inner cannulas must be reinserted before connecting to the ventilator circuit. If there was an inner cannula and it was removed, replace it with a clean inner cannula. The entire tracheostomy tube may need to be changed if replacing the inner cannula still does not allow the suction catheter to pass.
The National Tracheostomy Safety Project has an algorithm for Emergent Tracheostomy Management including cases where the suction catheter is unable to pass.
.
Open versus Closed Circuit Suctioning
Tracheal suctioning can be performed either with open circuit or closed circuit (Ballard) suctioning. Open suction catheters involve using singe-use catheters. Closed suctioning consists of a catheter enclosed in an outer plastic sheathe which allows the same catheter to be used multiple times. The closed suctions come in two lengths, one for an endotracheal tube and one shorter one specific for patients with tracheostomy. Closed suction catheters are usually changed every 72 hours or according to manufacturer instructions.
A comparison of open versus closed suctioning in individuals endotracheally intubated showed similar results in safety and effectiveness for rates of mortality and ventilator associated pneumonia (Sola, L & Bonito, S., 2007). Advantages of a closed circuit suctioning are ease of use and eliminating the need to disconnect the individual from the ventilator. Closed suctions add weight to the ventilator circuit.
Suctioning Procedure
Pre-suction procedure
Preparation for suctioning depends on an emergent versus a non-emergent need for suctioning. In cases of acute respiratory distress, where obstruction of the airway or the airway adjunct is suspected, suctioning must be performed emergently, with even minimal preparation. Care should be taken to maintain sterility while suctioning the endotracheal/tracheostomy tubes.
Once a need for tracheal suction has been established, the careprovider should make sure all equipment is available and functioning adequately.
Equipment needed for suctioning:
- A functional suction unit
- Sterile catheters
- O2 therapy – wall flow meter/portable bottle and tracheostomy mask
- Sterile water and bowl
- Yankauer suction catheter
- Personal protective equipment (gloves, gown as needed, ideally goggles/mask)
Prior to beginning the procedure, educate and explain the suctioning procedure to the patient. Suctioning can be anxiety provoking for the patient. An individual who is awake and cooperative may be asked to cough up secretions in order to limit suctioning and potential tracheal trauma. Tracheal damage and hypoxia can also be minimized by using an appropriately sized suction catheter. It is recommended that the external diameter of the suction catheter to be no more than half of the internal diameter of the tracheostomy tube. Larger catheters may cause damage or occlude the tube resulting in hypoxia. A catheter that is too small may not remove the secretions adequately or result in multiple attempts that can cause trauma to the airway.
Table: Approximate suction catheter size according to tracheostomy tube inner diameter
Infection control:
After explanation and consent, make sure to follow infection control procedures. Clean hands prior to placing gloves on. An apron should be worn to protect clothing and other patients. Consider a mask and goggles during the open suctioning technique, particularly if the patient has an infection or if there are copious secretions.
Patient positioning
Support the patient in a position that will facilitate coughing (unless contraindicated).
Suction pressures:
There is a delicate balance between effectively removing secretions and reducing injury to the tracheal mucosa. Suction pressure should not exceed -150 mmHg (-20kPa) and is appropriate for most patients. Higher pressures may result in trauma to the tracheal tissue or hypoxia from aspirating oxygen. Blood stained secretions may indicate tracheal injury. Large quantities of blood or persistent bleeding should be investigated to determine the cause of the bleeding.
Suction technique:
Pre-oxygenate the patient with 100% oxygen prior to suctioning to reduce the risk of hypoxemia. The catheter should be introduced to the desired depth. Do not apply suctioning while introducing the catheter as this can increase the risk of mucosal damage and hypoxemia. Occlude the suction port with a gloved thumb and suction upon removal of the catheter. Suctioning should be continuous, not intermittent. Intermittent suctioning does not reduce trauma and is less effective.
Depth of suctioning:
Shallow suctioning is when the suction catheter is passed to the tip of the tracheostomy tube. This technique is often used if the patient has loose secretions that are able to be coughed to the end of the tube. If the suction catheter is passed further than the end of the tracheostomy tube, this is considered deep suctioning. Deep suctioning may be required if shallow suctioning does not clear secretions adequately. For effective deep suctioning, many experts advocate advancing the suction catheter until the carina, where resistance is met. Once resistance is met, the suction catheter should be withdrawn slightly before suctioning is commenced.
Duration of suctioning:
Brief, 10-second suction duration is usually recommended to avoid mucosal damage and prolonged hypoxia. If there is a need for repeated suctioning, care should be taken to maintain and normalize vital signs in between suction episodes with special attention to the heart rate and oxygen saturation levels.
Upon completion of suctioning
When performing closed suctioning, the tip of the catheter should always be in the withdrawn position when not being used. The visible black marker indicates that the tube is withdrawn. Flush the closed suction tubing with clean water and empty the water receptacle as needed.
Reattach any oxygen to the patient if indicated. If using an open suction system for a patient receiving mechanical ventilation, reattach all equipment. If the patient has a fenestrated tracheostomy tube, the unfenestrated inner cannula must be in place before suctioning.
Summary
The adequacy of suctioning can be assessed by the clearance of secretions, improved breath sounds, improved air entry, good pulse oximetry readings, and improvement in respiratory distress in a patient. The importance of suctioning of both ventilated and non-ventilated patients with tracheostomy cannot be overstated. The presence of thick viscous secretions can lead to atelectasis, a decrease in oxygenation and even collapse of the lung lobe(s).
References:
Subirana M, Solà I, Benito S. Closed tracheal suction systems versus open tracheal suction systems for mechanically ventilated adult patients. Cochrane Database of Systematic Reviews 2007, Issue 4. Art. No.: CD004581. DOI: 10.1002/14651858.CD004581.pub2