Tracheostomy 101 for patients and families
Receiving news that you or a loved one may need a tracheostomy tube can be scary. How long will it be needed? What will life be like? Can you eat with a trach? Can you talk with a trach tube? These questions and more may arise. There can be many benefits of having a tracheostomy over intubation including reduced need for sedation, comfort, potential for voicing and eating/drinking. There are also some benefits of tracheostomy is the patient is not intubated including comfort, improved secretion management, possibly less trips to the hospital, improved breathing. The physician can discuss the patient’s individuals needs and potential reason for a tracheostomy.
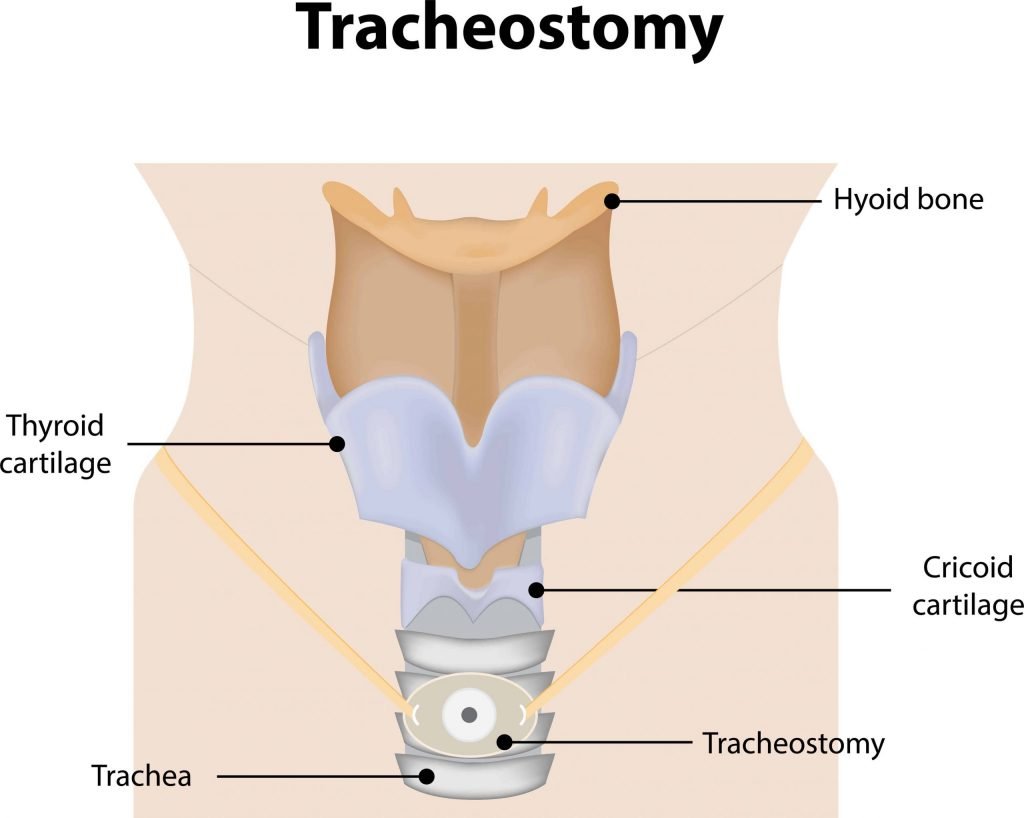
What is tracheostomy?
A tracheotomy is the surgical procedure where an opening in the neck (stoma) is made which is where a tracheostomy tube is then inserted. The tube is placed into the stoma and into the neck to allow air to enter directly into the lungs. After the tracheostomy tube is inserted, breathing occurs in through the tracheostomy tube and enters the lungs. On exhalation, air flows back out through the tracheostomy tube. For adults, a cuffed tracheostomy tube is usually the first tube to be placed which allows for positive pressure ventilation. In other words, it allows the ventilator to deliver breaths into the patient’s lungs directly with no escapage of air around the tracheostomy tube and through the upper airway.
When the cuff is inflated, the individual will not be able to voice. This is because air is needed to pass through the vocal folds for them to vibrate for voicing. Since no air passes through the vocal folds when the cuff is inflated, there will be no voicing. But person’s voicebox or vocal folds are still intact.
Can a person with a tracheostomy speak?
Yes, a person has the ability to produce voicing with a tracheostomy. The cuff of the tracheostomy tube would need to be deflated. However the patient needs to be medically stable before this can happen. The doctor will determine if the patient is medically stable for cuff deflation and an order is typically placed prior to attempts at cuff deflation.
Once the cuff is deflated there are a few different options for voicing including placing a gloved finger over the tracheostomy tube or using a speaking valve. A trained clinician such as a speech-language pathologist is typically the clinician to assess which communication option is the best and for the safety of speaking valves.
If the cuff cannot be deflated, options for communication include alternative communication (AAC devices), talking tracheostomy tubes, or the Blom Tracheostomy Tube system. It’s important to understand the options to bring these suggestions to your clinical team to help determine what’s best.
Can a person eat/drink with a tracheostomy?
Many individuals with tracheostomy also have dysphagia, or difficulty swallowing. When food or liquid goes into the airway (below the vocal folds) this is called aspiration. Aspiration can result in pneumonia, particularly in individuals with a medically complex history, such as many with tracheostomy. Those who are not safe for eating or drinking may have alternative means of nutrition such as feeding tubes such as nasogastric (NG), percutaneous gastrostomy (PEG). However, some people with a tracheostomy can safely eat or drink by mouth. It is important to be individually assessed for safety for eating and drinking by a trained clinician such as a speech-language pathologist.
How long will the tracheostomy be in place?
The length of time that someone has a tracheostomy depends upon the reason for the tracheostomy tube. Once the reason for the tube has been resolved, usually the tracheostomy tube can be removed (decannulated). Some individuals have the tracheostomy for a short period, even a few days, while others have the tube lifelong.
Summary
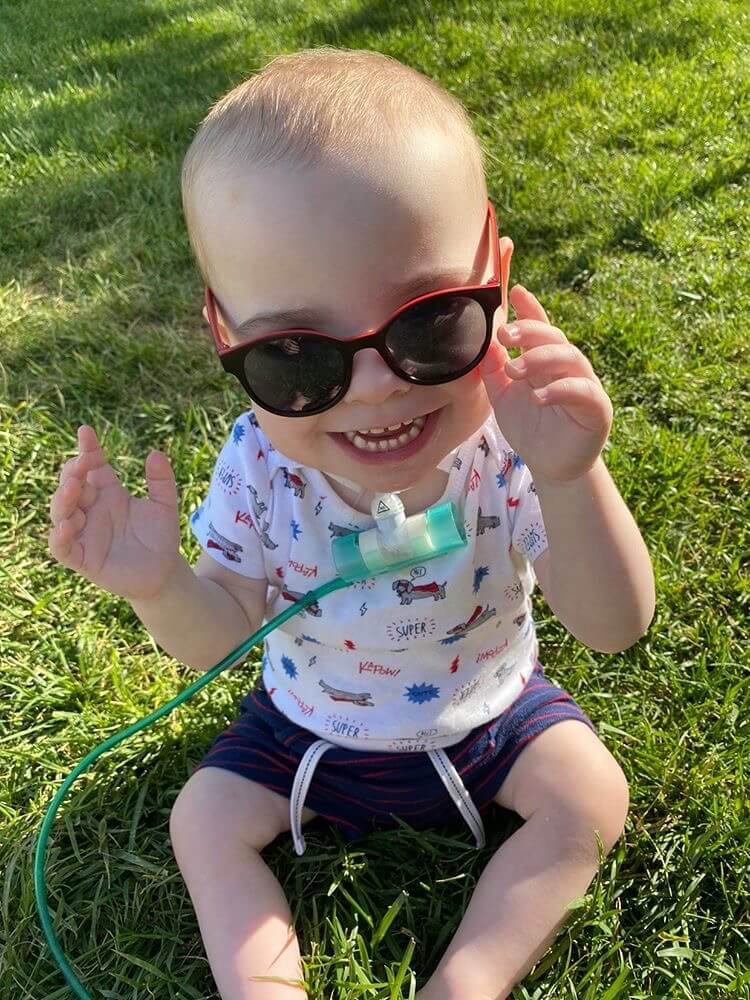
It’s important to speak to the healthcare team about the advantages and disadvantages of a tracheostomy. Having a tracheostomy tube can allow for the patient to possibly go home. Many patients live in the community with a tracheostomy tube.










Responses