Carter, A., Fletcher, SJ., Tuffin, R., The effect of inner tube placement on resistance and work of breathing through tracheostomy tubes: a bench test. Anaesthesia. 2013 Mar;68(3):276-82. doi: 10.1111/anae.12094. Epub 2012 Dec 20.
Cowan T, Op’T Holt TB, Gegenheimer C, Izenberg S, Kulkarni P. Effect of inner cannula removal on the work of breathing imposed by tracheostomy tubes: A bench study. Respiratory Care, 2001;46(5): 460–465.
Hernández G, Ortiz R, Pedrosa A et al. The indication of tracheotomy conditions the predictors of time to decannulation in critical patients. Med Intensiva. 2012;36(08):531–539. [PubMed] [Google Scholar]
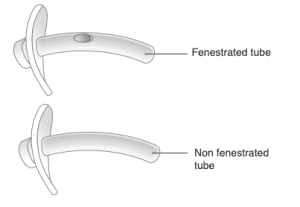
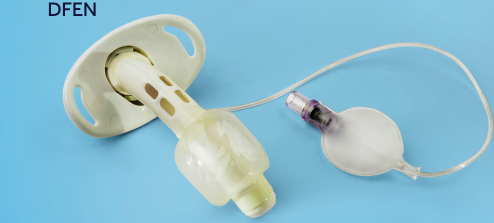
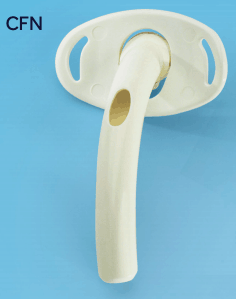
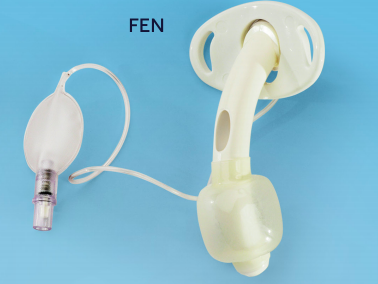
Hussey JD, Bishop MJ. Pressures required to move gas through the native airway in the presence of a fenestrated vs a nonfenestrated tracheostomy tube. Chest. 1996;110(2):494-497.
Khoo K, Arnot-Smith J. Complications with the use of Bivona adjustable flange tracheostomy tube. J Intensive Care Soc. 2015;16(1):81–82. doi:10.1177/1751143714552991
Mitchell, RB, Hussey, HM, Setzen, G, Jacobs, IN, Nussenbaum, B, Dawson, C., Brown, CA, Brandt, C., Deakins, K., Hartnick, C., Merati, A. Clinical consensus statement: tracheostomy care. Otolaryngology Head Neck Surgery, 2013;Jan;148(1):6-20.
Rumbak, M. et al. Significant Tracheal Obstruction Causing Failure to Wean in Patients Requiring Prolonged Mechanical Ventilation: A forgotten Complication of Long Term Mechanical Ventilation. Chest, 1999.
Shrivastava DK, Kapre S, Gray R. Weaning is facilitated by use of nonfenestrated tracheostomy tubes in chronically ill tracheostomized subacute care patients. Chest. 2003;124(4_MeetingAbstracts):205S