Emergency Equipment for Individuals with Tracheostomy

Emergency and Basic Equipment for Individuals with Tracheostomy
All clinical staff should be aware of the location of equipment for individuals with tracheostomy. Equipment should be kept at bedside in an easily accessible location for both routine and emergency use. When transferring an individual to a different location within a unit or to an outside unit, emergency equipment should also be available. All caregivers should be provided with a checklist of emergency supplies prior to discharge.
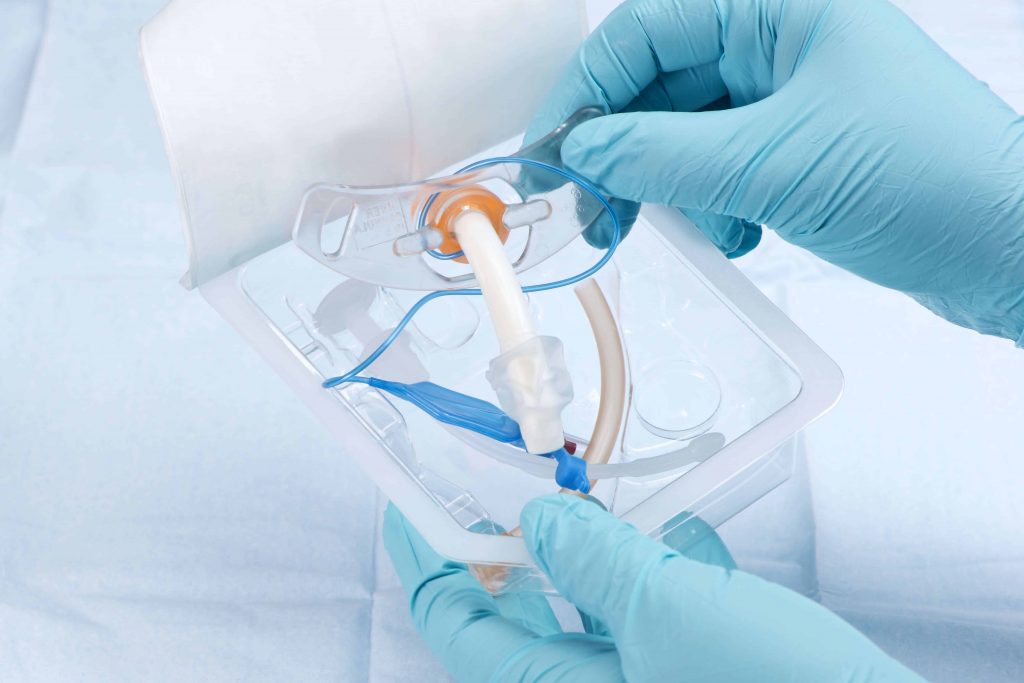
At a minimum a replacement tracheostomy tube of the same size and one of a smaller size should be available at bedside. An obturator is located in packaging. If the tracheostomy tube is cuffless, an additional cuffed tracheostomy tube is also recommended. Some tracheostomy tubes require an inner cannula to the ventilator circuit and in that case, a spare inner cannula should be at bedside. According to the Clinical Consensus Guideline “all supplies to replace a tracheostomy tube should be at bedside or within reach (Mitchell, 2012).
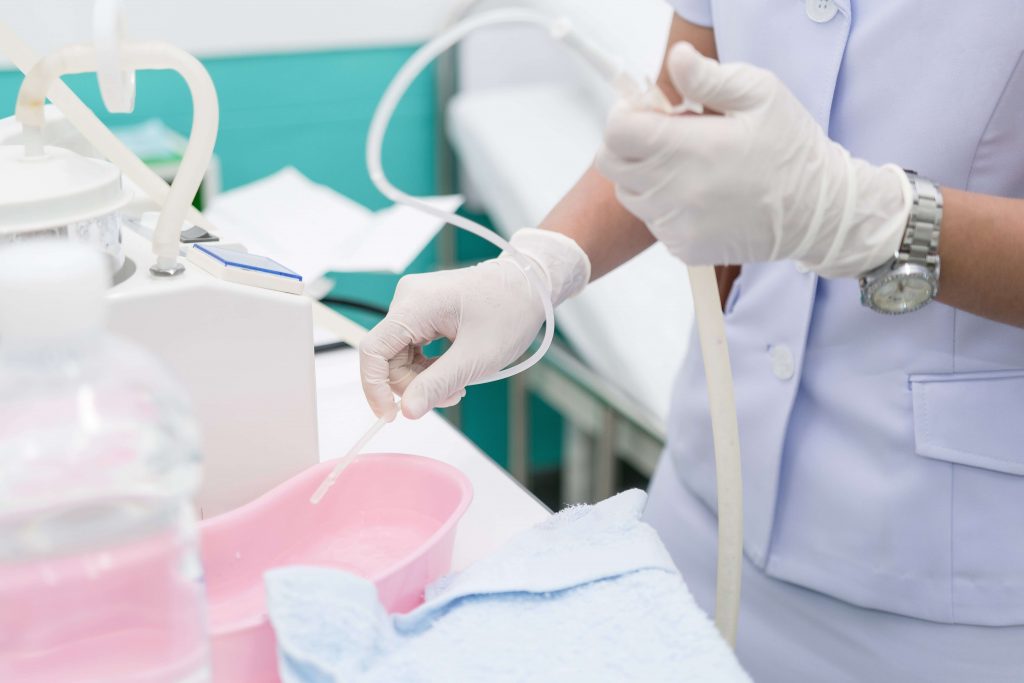
Flexible suction tubing and suctioning aparatus should be at bedside. A range of suctioning catheter sizes should be available at the facility with the appropriate size at bedside. Check the manufacturer recommendations for appropriate suction catheter size for the inner diameter. A general guideline is below.
An Ambu bag or a bag valve mask (BVM) should be with the patient at all times in case of emergency.
Advanced airway equipment such as laryngeal mask airways (LMAs) and a range of endotracheal tube sizes should be available on an arrest trolly cart. A small size 6.0 endotracheal tube should be available as this can be inserted into the stoma if necessary.
Oxygen masks for the tracheostomy and face should be available. Laryngeal mask airways and pediatric airways can be used to oxygenate and ventilate the stoma and should also be available for all patients with tracheostomy. Oral and nasal airways should also be available.
A fiberoptic endoscope should be available in any area caring for patients with tracheostomies. Immediate availability is required for critical care and other specialist areas, where endoscopes can be used to inspect tubes suspected of being displaced, or to guide the insertion of bougies or tubes into stomas.
Some clinicians find stock dilators essential to keeping the stoma open or manipulating the tracheostomy into the stoma. Having a dilator at bedside is a facility based decision.
Bougies can help with routine tube changes or re-insertions. During an uneventful tube change, the tracheostomy tube starts in the trachea and therefore the bougie will likely remain in the trachea as it is inserted. However, if the tube is displaced because a bougie is stiff, blindly inserting a bougie into the stoma may result in a false passage being formed. It is safer to use either a fibre-optic endoscope or a hollow bougie loaded onto a ‘scope for this purpose. Blind insertion should be avoided if at all possible.
PPE is used to protect the careprovider as well as the patient in preventing the spread of infection. Gloves should be donned at all times during tracheostomy care. Other protective equipment such as an apron or eye protection are worn as needed depending on location and infection status.
A 10ml syringe is important at bedside in order to deflate the cuff (if present) of the tracheostomy tube. The cuff must be deflated for tracheostomy tube changes and therefore quick access to a syringe is important in emergency situations.
Scissors are important to remove tracheostomy tube ties and dressings quickly during an emergency.
Other equipment includes water soluble lubricating jelly, tracheostomy tube ties and dressings. The water soluble lubricating jelly is for easier placement of the tracheostomy tube during insertion.
Emergency bed head signs such as these from the National Tracheostomy Project are also recommended for emergency to distinguish between tracheostomy and laryngectomy in an emergency.
Suction catheter sizing chart
Here is an emergency algorithm for tracheostomy from the National Tracheostomy Safety Project- http://www.tracheostomy.org.uk/storage/files/Patent%20Airway%20Algorithm.pdf
Pediatric bedside equipment
Recommended pediatric bedside equipment:
- Spare tracheostomy tube (same size) plus tapes
- Half-size smaller tracheostomy tube plus tapes
- Round-ended scissors
- Spare tapes
- KY Jelly
- Syringe and saline
- Suction catheter
Basic (face masks, airway adjuncts, supraglottic airway devices) and advanced equipment (laryngoscopes and endotracheal tubes) to manage the upper airway must be available on a resuscitation trolley for hospitalized patients.
Emergency Training
Clinicians should be trained in emergency scenarios when working with patients with tracheostomy. Patients and careproviders caring for those with tracheostomy should also be trained prior to discharge. A tracheostomy simulation can help with training to provide different scenarios for patients. A Tracheostomy Manikin such as the Tracheostomy Trainer can help to educate where the learner can be provided with different scenarios such as tracheostomy changes, inner cannula changes, mechanical ventilation and alarm scenarios, suctioning and other tracheostomy care.
Summary
Clinicians must be prepared in case of emergency as the medical condition of a patient with tracheostomy and/or mechanical ventilation may change quickly. Emergency equipment is necessary at the bedside as well as during trasportation.