Tracheostomy Awareness May 16th through 22nd, 2021

Tracheostomy Awareness Week has a goal of raising awareness of tracheostomy patients and their families. Tracheostomy Awareness initially began with a parent of a child with tracheostomy. Parents of kids with tracheostomy can be powerful advocates for their children. We have seen many amazing success stories and incredible love. At Tracheostomy Education our mission is to spread awareness of tracheostomy and to improve the safety, care and lives of those with tracheostomy.
In the past year, there has been an increase in patients requiring mechanical ventilation due to Covid-19. Some individuals with severe respiratory distress required prolonged mechanical ventilation and benefited from tracheostomy tube placement. Here is more information about Covid-19 and tracheostomy.
This year for Tracheostomy Awareness 2021, parents of children with tracheostomy and patients have provided information on what it’s like to live and thrive with a tracheostomy. These courageous families have shared a part of their lives with us in order to help others.
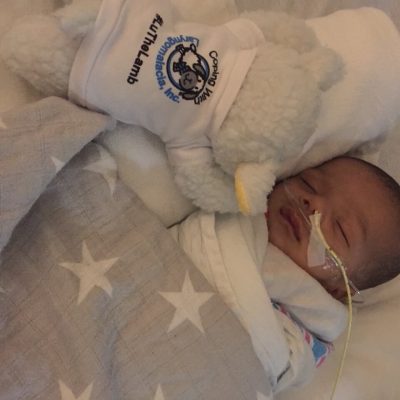
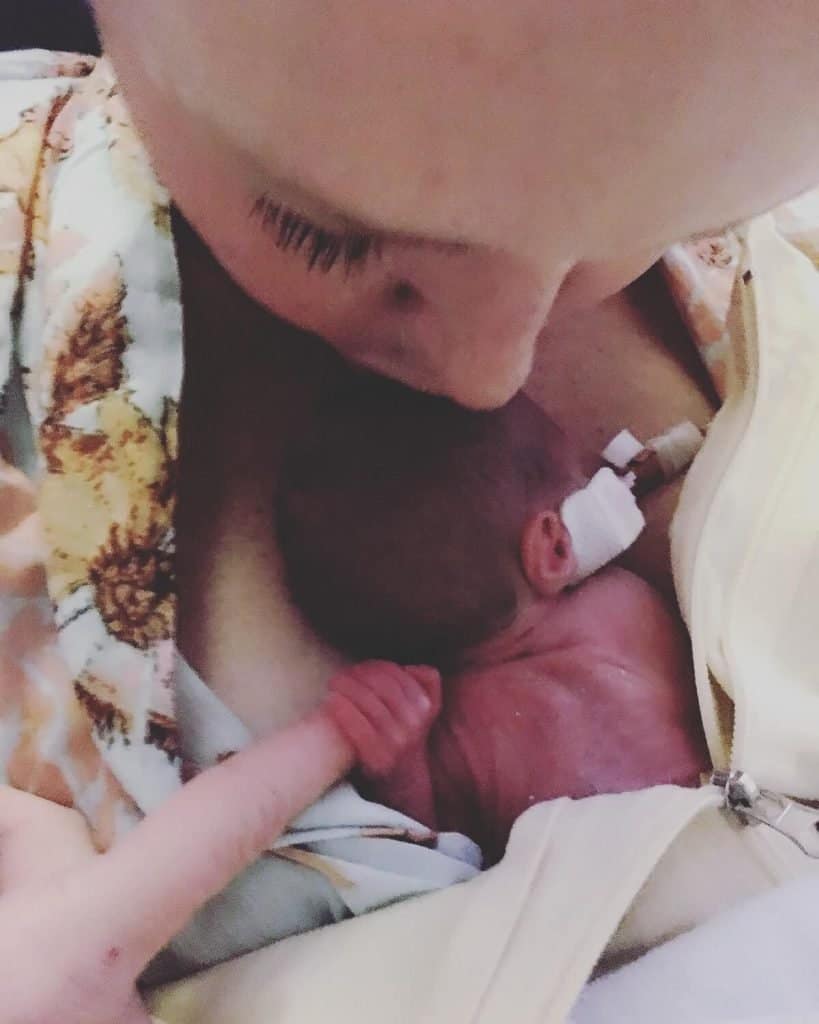
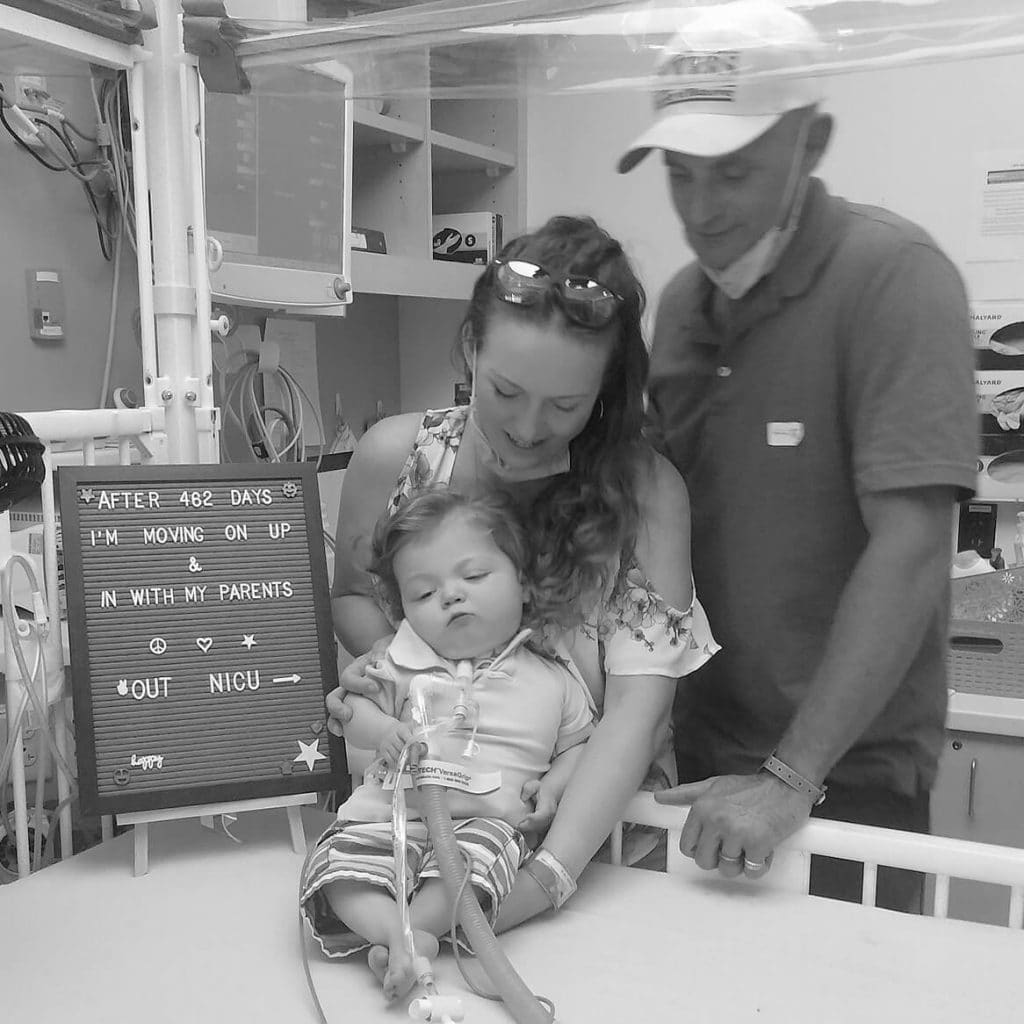
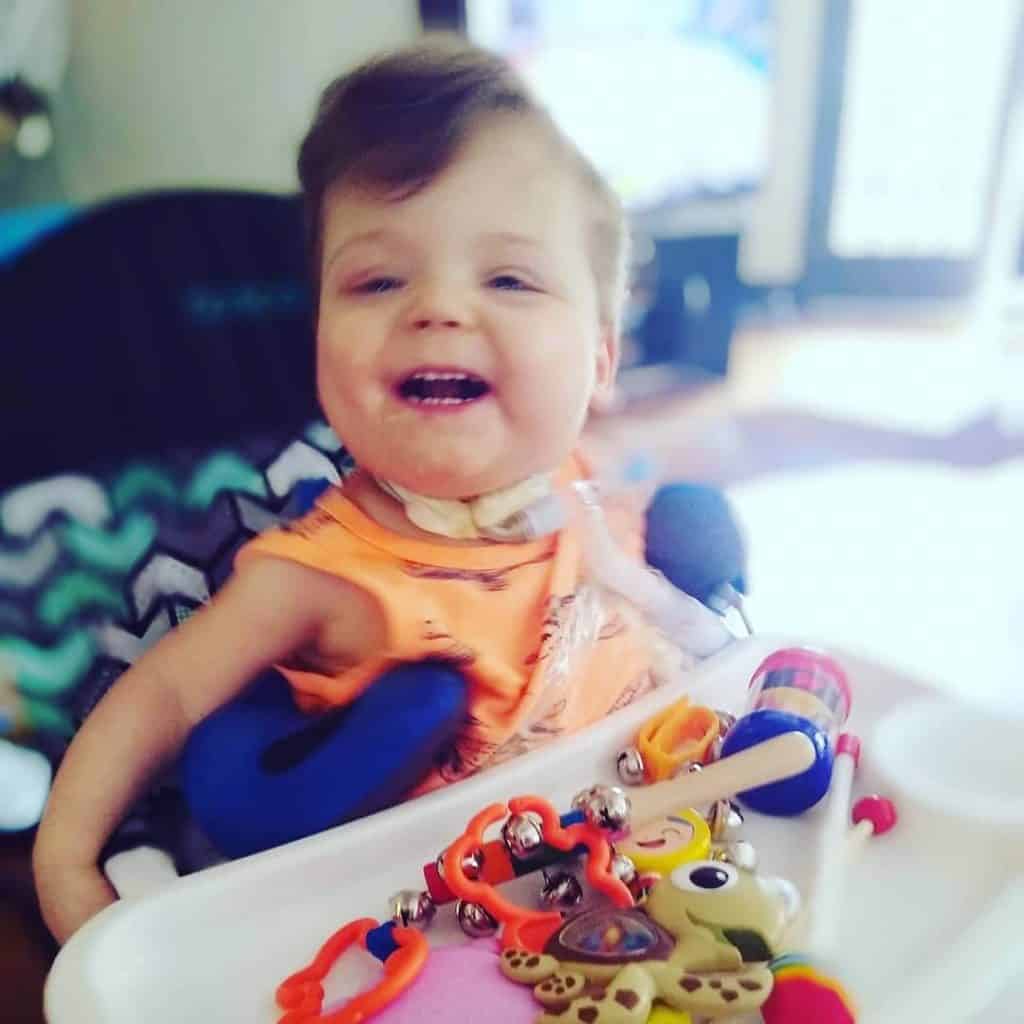
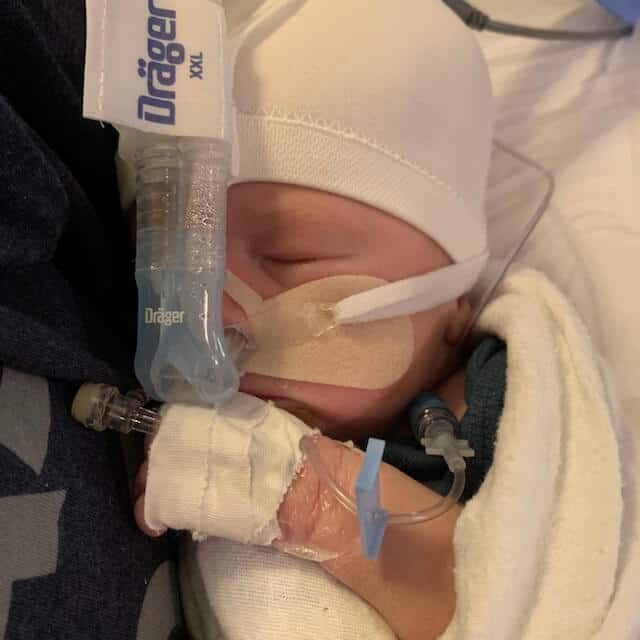
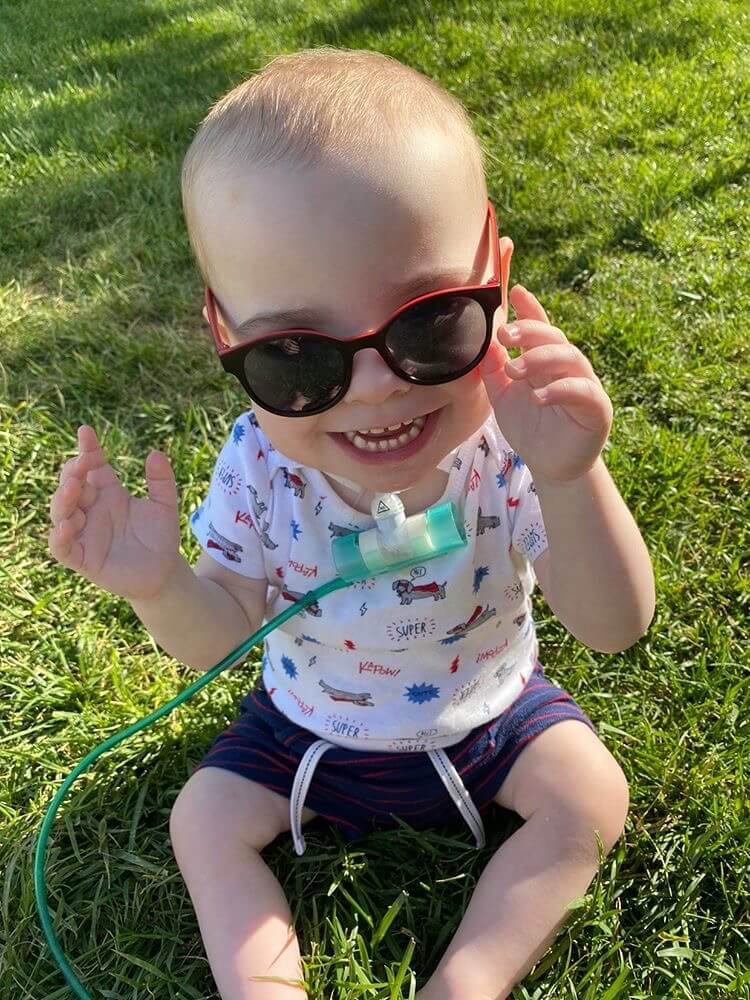
My name is Tasha.. My sons name is Phoenix & was born a micro-preemies weighing 1 lb 7oz’s, 3.5 months early due to placental abruption. He had severe bpd due to his underdeveloped lungs which was our reason for getting trached. We spent his whole 1st year of life in the NICU, 462 days to be exact. My husband & I were so hesitant to move forward with the tracheostomy at first.. We waited as long as we could to give him time to be a candidate for extubation if he improved… After lots & LOTS of prayer we moved forward with surgery on Sept 17th, 2019 1 month after my husband & I got married in the NICU at the foot of his hospital bed & have been so pleasantly surprised to see that it has done the opposite of what we feared it would do… It hasn’t limited his quality of life it’s GIVEN him quality of life.. A common misconception I think most trach parents have at first. Anyhow he will be turning 2 on May 6th & are ecstatic to celebrate our 2nd bday, but 1st bday AT HOME❤️
Thanks so much for taking time out to learn about our little fighter.. He is our HERO.
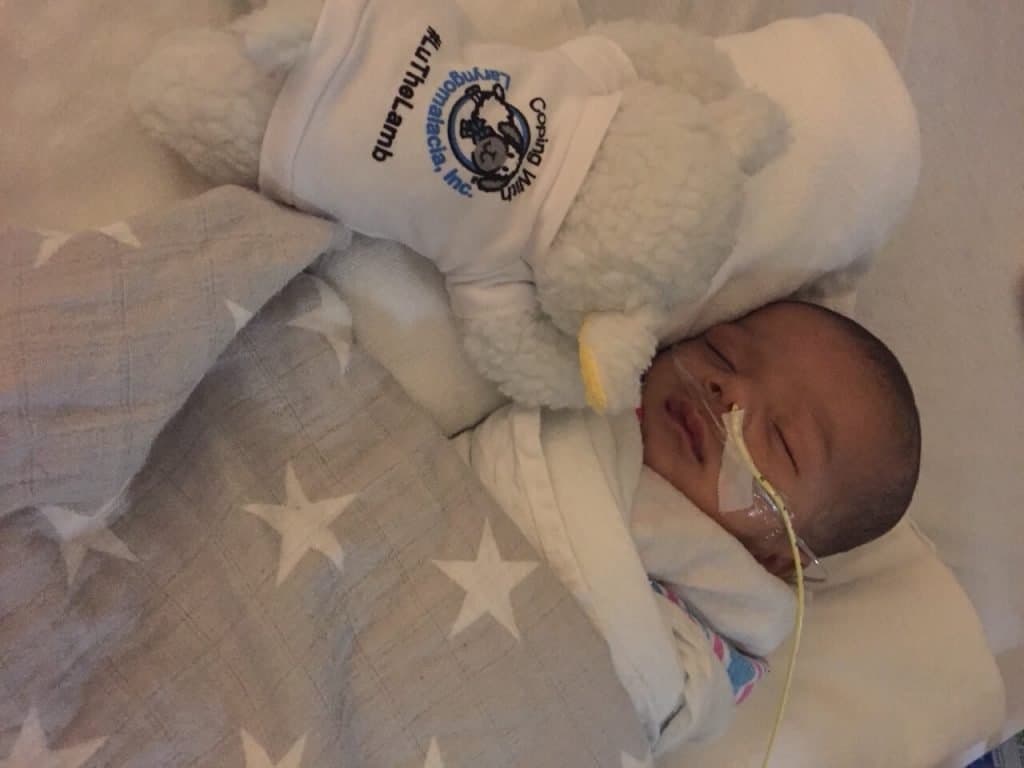
Easton was born 10/2019.
He spent 167 days in the NICU, in charleston, sc. He was diagnosed with a rare neuromuscular disease called Congenital Myasthenia Syndrome. CMS creates difficulties when it comes to breathing, and airway challenges such as paralyzed vocal cords, and larayngomalasia. Due to these challenges, the best way to ensure EP (as he’s lovingly called) to go home was to have a tracheotomy surgery. The training on how to care with a child with a trach took several weeks, and to be brutally honest it is scary at first. Quickly Easton began to recover, and his parents saw the trach was the best decision for him. Finally after 5 months apart the entire family was reunited.
Easton has now had his trach for a little over a year. It has helped him to thrive at home. He has wonderful caregivers, and siblings who have all learned so much about being medically complex. Yet the number one thing we have all learned is to be grateful for medical advances.

When my daughter Isabelle was 6 months old, she wasn’t progressing with her breathing in the nicu. When we made the very hard decision to get a tracheostomy, my husband initially thought they would cut through the vocal cords and we would never hear her voice. We also didn’t think we would be able to do anything outside of the home, ever. The big picture was just very scary when you have no idea! I believe the biggest benefit to us regarding Isabelle’s care is the education that the hospital had given us before she came home. We had to do a lot of hands on learning, care of the trach site and neck, and multiple trach changes before she was able to come home. This part of the process took away much of the fears we were experiencing and answered questions. We learned how to be our child’s nurse. Your education as a parent is more beneficial than the education the LPN’s receive. Often times our nurses tell us that they learned more from us than their education. Even the few times we had an emergency and panicked and called 911, paramedics would be clueless as to what to do and stand there watching us in action.
Honestly, caring for a tracheostomy isn’t as scary as the hospital makes it to be. It’s their job to scare you so you know what to do in every single situation. Will you go through all of those situations? Nope!
My child became a completely different child as soon as she got home. Watching your child learn new things or wean down on breathing requirements is the most amazing feeling. And it’s all because of what you do for them!
Also, Social media is an extremely wonderful way to see what every family does differently! We share thoughts and ideas, offer advice or just lend a listening ear. You don’t HAVE to feel alone! Having a great support system is so important.
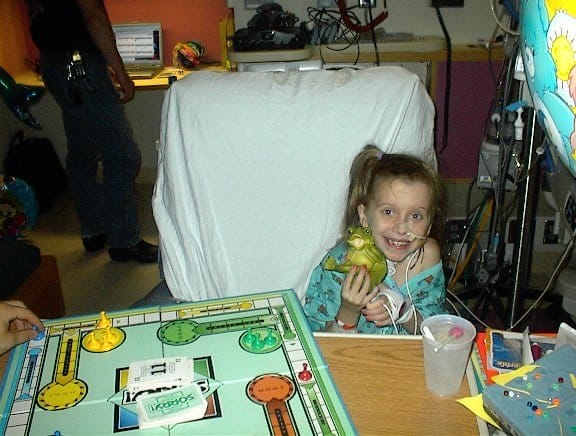
Hi my name is Melissa also known as realmelissa from Instagram I was a former passy valve tracheotomy patient in 2005 at Mayo Clinic in Rochester Minnesota. I stayed at Saint Mary’s hospital when I was 6 years old back then here is some photos of when I was 6 years old I’m 23 years old now.
Kylie was born full term at 38W5D with 7.5lbs. She was immediately sent to NICU since born with suspected Transient tachypnea of the newborn (TTN).
Doctor slowly diagnosed her underlying medical conditions : Likely Pierre Robin Sequence and cleft palate.
Hence she was intubation at birth in view of poor respiratory effort. She was little warrior that fight to live, she was given the chance to breathe on her own after two extubations on Day 2 of birth and Day 16 of birth respectively, but she just get too tired even though she was on CPAP and BPAP. She had bad chest recession.
In view of poor respiratory, tracheostomy is the only option for her according to doctor. She was trach when she was 3W5D old due to upper airway obstruction secondary to glossoptosis and retroflexed epiglottis. Immediately after the tracheostomy procedure, she looks so much comfortable and good saturation.
Kylie is now 9 months old now, she’s just a little cheeky baby with lovely smiles. She’s growing happily and healthily.
All I want to say is that tracheostomy is the wise choice for Kylie because it gives her life. It also give us, as parents to look after Kylie. It’s challenging journey but a meaningful one.
Btw, we are located in Kuala Lumpur, Malaysia 😉
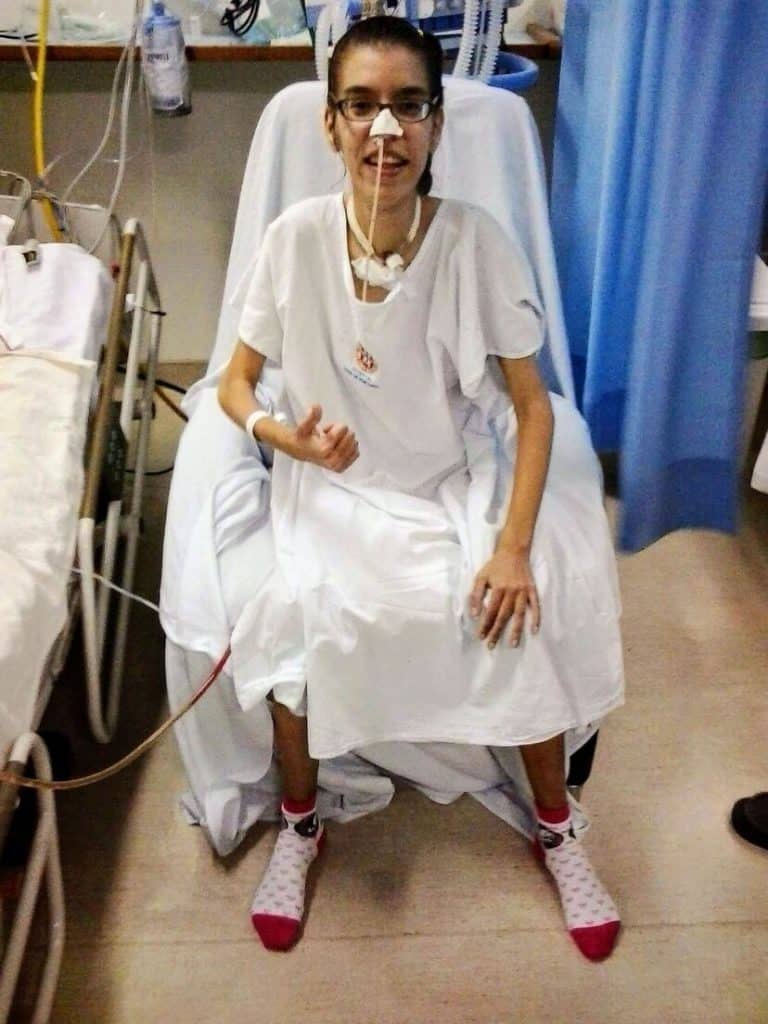
My name is Lorrayne, I live in Rio de Janeiro, Brazil and I’m 30 years old.
Aged 1 and under, I was diagnosed with a type of dystrophy, minicore myopathy.
As this disease has no cure, it is very important to do physical therapy to maintain movements. I was able to walk until I was 23 years old. But, in 2014, pneumonia worsened my condition and I ended up having respiratory failure.
In May 2014, the tracheostomy entered my life, after 5 days of intubation. It keeps me safe in the respiratory area today and it will probably be like this forever.
But, I manage to have a happy life even with the tracheostomy. I found myself in the art of Lettering and today I share my art bringing joy, inspiration and love to people.

Meet Zack, born on April 11, 2019, from UAE, Dubai, suffered severe loss of oxygen to his brain and diagnosed with severe HIE. He received his tracheostomy at only 2 months old, but did not expect him to live long, but God had other plans.
Everyday is still a learning curve for us. At first we did not touch his trach and was so scared but it has been almost a year that we’ve been changing his tracheostomy tube at home.
We are proud of our boy and proud to be Trach Parents. Zack just turned 2 on April 11, 2021.
If you would like to be included on the site, please email [email protected] or DM us on instagram @tracheostomyeducation
Tracheostomy Awareness Gifts
All proceeds from the gift store go directly into the website Tracheostomy Education to educate patients and clinicians on tracheostomy.
-
 Feeding Management for Infants with a Tracheostomy
Rated 0 out of 5$35.00
Feeding Management for Infants with a Tracheostomy
Rated 0 out of 5$35.00 -
 Chronic Respiratory Failure in Tracheostomy Dependent Children: An Overview
Rated 0 out of 5$35.00
Chronic Respiratory Failure in Tracheostomy Dependent Children: An Overview
Rated 0 out of 5$35.00 -
 Tracheostomy Training In-Person MasterClass 2024
Rated 0 out of 5
Tracheostomy Training In-Person MasterClass 2024
Rated 0 out of 5$550.00$497.00 -
 Tracheostomy Care for Adults: Basics and Troubleshooting
Rated 0 out of 5$40.00
Tracheostomy Care for Adults: Basics and Troubleshooting
Rated 0 out of 5$40.00 -
 Adult Decannulation Webinar: Evaluating and Treating the Upper Airway
Rated 0 out of 5$95.00
Adult Decannulation Webinar: Evaluating and Treating the Upper Airway
Rated 0 out of 5$95.00


















Responses